What is Osteonecrosis of the Knee?
Osteonecrosis is a condition in which the death of a section of bone occurs because of lack of blood supply to it. It is one of the most common causes of knee pain in older women. Women over 60 years of age are commonly affected, three times more often than men.
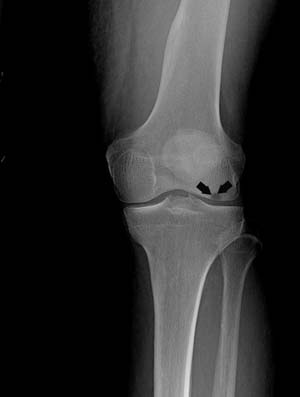
Osteonecrosis of the knee is most commonly seen in the medial femoral condyle, a projection of the lower end of the femur (thigh bone) present towards the inner side of the knee. The condition can also occur on the outside of the knee (the lateral femoral condyle) or on top of the shinbone (the tibial joint surface), known as the tibial plateau.
Causes of Osteonecrosis of the Knee
The exact cause of osteonecrosis of the knee is unknown. However, one of the theories suggests that a stress fracture or trauma can result in altered blood supply to the bone. Another theory says that fluid buildup within the bone increases the pressure on the blood vessels, resulting in decreased circulation. If the condition is not diagnosed and treated early, it can result in severe osteoarthritis. Certain conditions that are associated with osteonecrosis of the knee include obesity, sickle cell anemia, lupus, kidney transplants, and steroid therapy. Steroid-induced osteonecrosis affects multiple joints and can be seen in younger patients.
Symptoms of Osteonecrosis of the Knee
Osteonecrosis in the knee results in the sudden onset of pain inside the knee, which is triggered by a specific activity or minor injury. The pain worsens with activity and at night. Osteonecrosis may also cause swelling of the knee and sensitivity to touch and pressure and can result in limited motion due to pain and swelling.
There are four stages of development, which can be distinguished by symptoms and X-ray results.
- Stage I: The symptoms are most intense in the earliest stage, and may subside in 6 to 8 weeks. The X-rays are normal. A positive bone scan may be required to make the diagnosis. Treatment is by non-surgical methods that focus on relieving pain and weight-bearing.
- Stage II: This stage follows in a couple of months and the X-rays show flattened edges of the once rounded thighbones. An MRI, CT or bone scan would be helpful to diagnose the condition.
- Stage III: At this stage, the condition becomes clearly visible on X-rays and no other diagnostic tests are required. At this point, the bone itself begins to decay and cartilage covering the bones loosens from other segments of the leg. Surgical treatments are considered at this stage.
- Stage IV: In this stage, the articular cartilage is destroyed, joint space narrows, bone collapses, and bone spurs form. The only treatment at this point is joint replacement surgery.
Treatment of Osteonecrosis of the Knee
In the early stage of the disease, non-surgical treatment options are suggested, including anti-inflammatory medications, braces, strengthening exercises for thigh muscles, and activity modification, to reduce the knee pain.
Surgical treatment is considered in advanced stages where more than half of the bone surface is affected. Surgical treatment options include:
- Arthroscopic debridement or cleansing of the joint
- Drilling the area of osteonecrosis of the knee to decrease pressure on the bone surface
- Procedures to lessen the weight on the affected area
- Unicompartmental or total knee replacement
Your doctor will discuss all the surgical options and recommend the most appropriate one for you.
Related Topics:
- Chondromalacia Patella
- Baker's Cyst
- Iliotibial Band Syndrome
- Knee Injury
- Unstable Knee
- Knee Sprain
- Knee Infection
- ACL Tears
- Multiligament Instability
- Knee Arthritis
- Chondral or Articular Cartilage Defects
- Osteonecrosis of the Knee
- Knee Angular Deformities
- Periprosthetic Knee Fractures
- Bowed Legs
- Knee Osteoarthritis
- Periprosthetic Knee Infection
- Knee Pain
- Anterior Knee Pain